What How Upper Cervical Chiropractors Help Neurodegenerative Disorders
The connection between upper cervical chiropractic care and neurodegenerative disorders is relatively shocking and many people may not know that upper cervical care can help. This blog will highlight how an upper cervical chiropractor can help you. Schedule a consultation today!
What is the connection between Upper Cervical Care, Parkinson’s, Parkinsonism pathologies, and other neurodegenerative disorders?
Many people are aware that our brain is bathing in a fluid that helps protect it from bumping into the skull walls. This fluid is called Cerebrospinal Fluid or CSF. CSF also has another vitally important function, which is to help facilitate the transfer of oxygen and nutrients to the neurons of the brain and spinal cord. However, many people are unaware that the blood vessels that go into the skull do not actually directly circulate to the brain and spinal cord; there is a special barrier that filters the oxygen and nutrients out of the blood, called the Blood Brain Barrier (BBB). The BBB actually helps keep many toxins and more importantly foreign invaders like bacteria out! This barrier is also the exit point for waste and toxins that we need to get away from the brain and spinal cord. (1)
Cerebrospinal Fluid is also very unique in that it moves and circulates around the brain and spinal cord on its own rhythm, distinctly different than the rhythm and circulation from the heart. In the cardiovascular system, the heart is the engine that pumps blood through the body. CSF is pumped via the biomechanical motion of the sacrum in your pelvis, and sphenoid bone of the skull. This top top-to-bottom pumping action keeps CSF flowing around the central nervous system. The equilateral flow of the CSF is essential to keeping all of the neurons in the brain and spinal cord healthy.
How can Chiropractic Care Help?
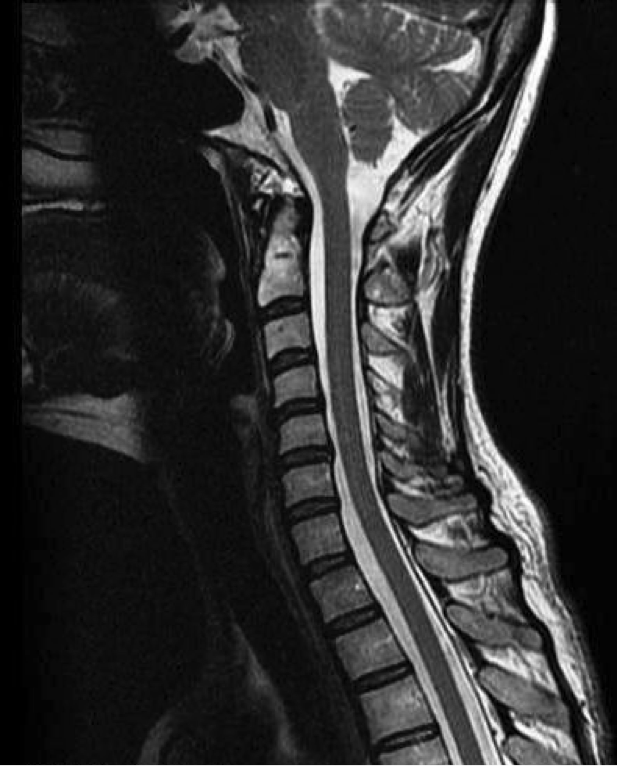
So, how is chiropractic, and specifically upper cervical chiropractic connected to CSF flow? In general, spinal misalignments and postural abnormalities can impede proper CSF flow in the spinal cord. This impedance can be acute, like after a major trauma such as whiplash, or chronic, with spinal misalignments accelerating degeneration of the spinal discs and bones, allowing bone spurs to form which create a speed bump-like obstruction in the area of the spinal cord flows, as seen in the picture below.
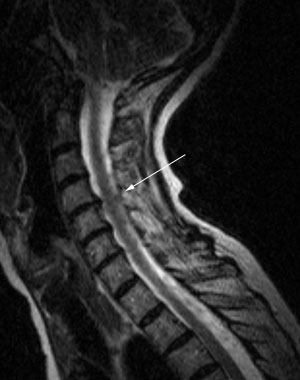
How Can Upper Cervical Chiropractic Help Specifically?
However even more significant, is the alignment in the upper cervical spine. A misalignment of the C0-C1 and C1-C2 vertebrae can impede CSF flow between the brain and spinal cord, making it much more detrimental to overall flow, and therefore health of the entire nervous system. More like a roadblock than a speed bump. This can then lead to an increase in the quantity of CSF in the cranium, which can increase the cephalic pressure, known as hydrocephalus. (1) Dr. Scott Rosa is a renowned Upper Cervical Chiropractor and researcher. Much of his research is done especially on CSF flow, upper cervical alignment, and advanced imaging. His studies show how an upper cervical misalignment affects flow and alters patterns of flow and pressure and fluid accumulations within the skull and brain. (2)
So what? Well, altered flow, decreases CSF nutrients and oxygenation, as well as increases intracranial pressures, potentially leading to hydrocephalus. There is a connection between CSF quality, hydrocephalus, and neurodegenerative disorders such as Dementia, Alzheimer’s, and Parkinson’s. A recent study found that Alzheimer-type and multi-infarct dementia syndromes were found more frequently in communicating hydrocephalus(3). The Mayo Clinic states that with hydrocephalus, the symptoms in older adults are almost identical to the symptoms of Parkinson’s with a shuffling gait, poor balance, memory loss, and more. Yet the events that lead up to the cause of hydrocephalus (which is an imbalance of CSF flow and production) in the medical profession are “unknown”(1), this is because typically medical doctors do not evaluate upper cervical spinal alignment…but check out this video shared by a MD with a mutual patient of Dr. Rosa where you can see the improved CSF flow after a specific upper cervical adjustment!!
Upper Cervical chiropractors like myself and Dr. Rosa specialize in the analysis and correction of upper cervical misalignments. This is done with a thorough x-ray analysis and a specific adjustment, that is gentle, with no twisting, popping, or cracking of the spine. We can help patients improve spinal alignment in the upper cervical area and the entire spine, therefore helping regulate and restore ideal CSF flow.
What Can You Do?
Worried this could be a problem for yourself or a loved one? If you have a family history of neurodegenerative disorders I would strongly recommend getting your spine examined, and misalignments corrected if needed. If you are in my practice area the first step would be to come into our practice for a consultation and your initial Neuro-Structural Testing. This is a non-invasive way to test your nervous system and see if you have any spinal misalignments, where they are in your spine, and how severe they are. After getting evaluated, if indication is present I will recommend the necessary very low dose digital x-rays for the N.U.C.C.A and Pierce Results System Spinal Structural and Functional analysis to identify how to best correct any misalignments that are identified.
References:
1) Hydrocephalus. https://www.mayoclinic.org/diseases-conditions/hydrocephalus/symptoms-causes/syc-20373604
2) Smith FW, Dworkin JS (eds): The Craniocervical Syndrome and MRI. Basel, Karger, 2015, pp 48-66: The Craniocervical Junction: Observations regarding the Relationship between Misalignment, Obstruction of Cerebrospinal Fluid Flow, Cerebellar Tonsillar Ectopia, and Image-Guided Correction
Rosa S. Baird J.W.
3) Disturbances Of Cerebrospinal Fluid (CSF) Circulation–Neuropsychiatric Symptoms and Neuroradiological Contribution.
E Hofmann-T Becker-J Meixensberger-M Jackel-M Schneider-H Reichmann – https://www.ncbi.nlm.nih.gov/pubmed/8579810
